
The use of electronic Health Records (EHR) systems is no longer a luxury in the contemporary medical care provision. They form the backbone of operational success of clinical documentation, patient coordination, billing, compliance and more and more, interoperability. Most of the debates of EHRs are on its pros and cons, but there is more strategic analysis of how an EHR can be integrated with other clinical technologies with standardized APIs and interoperability structures.
The EHR system is not just a documentation efficiency tool, but has a massive potential to be shared, interpreted, and synchronized with other imaging systems, laboratories, billing sites, and external providers; this is one of the most real values of a digital strategy within the healthcare setting when considered long-term.
This article focuses on the operational advantages and disadvantages of the EHR systems - and discusses the importance of such an interoperability standards, like HL7, FHIR and DICOM, in enabling sustainable healthcare IT architecture.
• Ehr Systems Enhance The Efficiency Of Documentation, Availability Of Patient Data, And Clinical Coordination, But The Costs Of Implementation And Workflow Disorientation Are Significant Issues.
• Interoperability Capability Is More Important To The Long-term Value Of An Ehr Than Documentation Features Alone.
• Integration Failures Are Usually Caused By Vendor Lock-in And Restricted Access To The Api.
• Hl7, Fhir, And Dicom Are Among The Standards That Determine Whether An Ehr Can Be Used Effectively To Exchange Structured Clinical And Imaging Data.
• The Current Healthcare Infrastructure Is Moving Towards Api Integration Rather Than Traditional Interface Engines.
• The Ehr Practices That Are Conducted To Evaluate Ehr Platforms Should Determine Integrative Preparedness And Usability, As Well As Costs.
An EHR system is an electronic platform developed to store and manage patient health information within the care setting. In contrast to traditional EMRs (Electronic Medical Records), which are usually limited to the records of a single provider, EHR systems are designed to help share data across organizations.
Functional modules usually consist of:
• Clinical Documentation
• Order Entry (cpoe)
• Management Of Laboratory And Imaging Results.
• Eprescribing
• Integration Of Billing And Revenue Cycle.
• Patient Portals
• Reporting And Analytics
Technically, advanced EHR devices are centralized data stores that are accessible via APIs and messaging standards. Whether the EHR stores data effectively or not is not the question of architecture - it is whether that data can be transferred across the systems in a seamless, structured, and standardized manner.
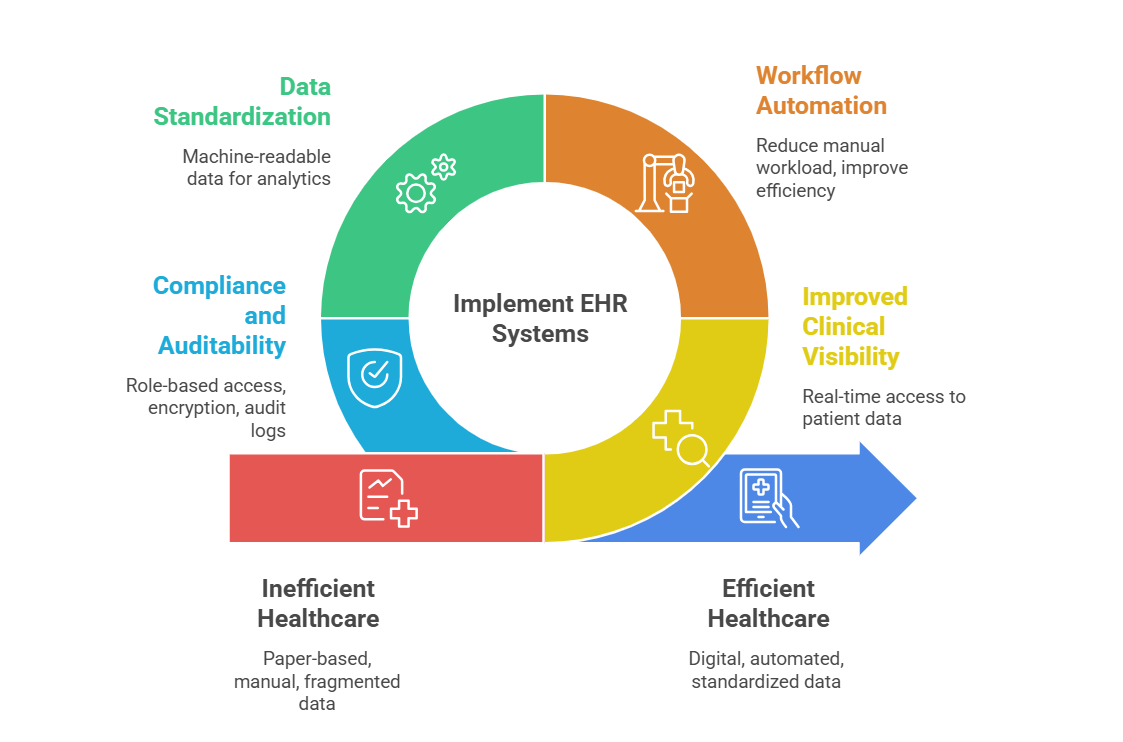
Electronic records minimize the use of paperwork systems and enable providers to obtain patient history, diagnostic outcomes, and past encounters instantly. This helps eliminate test overlap and facilitates clinical judgment.
Embarked charts, electronic prescriptions, and billing will minimize the workload and administrative overhead. Documented code is also better in enhancing accuracy.
Contemporary EHRs organize patient data in computer-readable formats. This enables:
• Quality Reporting
• Clinical Analytics
• Public Health Data Exchange
• Ai-assisted Diagnostics
Structured data would be exponentially valuable for interoperability with other systems.
Access controls, encryption, and audit records enable regulatory compliance and lower legal risk. Well-set-up EHR systems increase accountability and traceability.
EHR adoption is associated with measurable challenges, even though its advantages are evident.
The cost of implementation will consist of:
• Licensing Fees
• Hardware Upgrades
• Training Programs
• Workflow Redesign
• Ongoing It Maintenance
Integration costs- especially when relating to imaging systems or third-party software can be higher than estimated initially.
In implementation stages, productivity tends to reduce. Employees also need to be trained, and resistance to change can affect morale and productivity.
Other EHR vendors are closed-ecosystem vendors that do not allow the flexibility of external integration. Long-term scalability may be constrained by a proprietary API or a lack of interoperability framework.
The process of switching over legacy systems may include:
• Data Mapping Challenges
• Structured Consistency Is Lost.
• Downtime Risk
• Validation Requirements
These difficulties outline the importance of interoperability capability being considered when it comes to selecting a vendor
Interoperability defines how an EHR can be used as a network-based entity.
1. Foundational Interoperabilitybasic Data Transfer Not Interpreted.
2. Structural Interoperabilitydata In A Standardized Format, To Maintain Structure (e.g., Hl7 Messaging).
3. Semantic Interoperabilitysystems Make Sense Out Of Exchanged Data (e.g., Standardized Terminology).
The real efficiency in healthcare entails the three levels.
Messaging protocol widely used for the transmission of clinical data, such as admission, discharge, and order messages, between systems.
An open-source, REST-based API standard aimed at web-friendly healthcare integration. With the aid of the FHIR standardized resources (such as):
• Patient
• Observation
• Diagnosticreport
• Imagingstudy
FHIR supports complex integration over legacy HL7 messaging by a large margin.
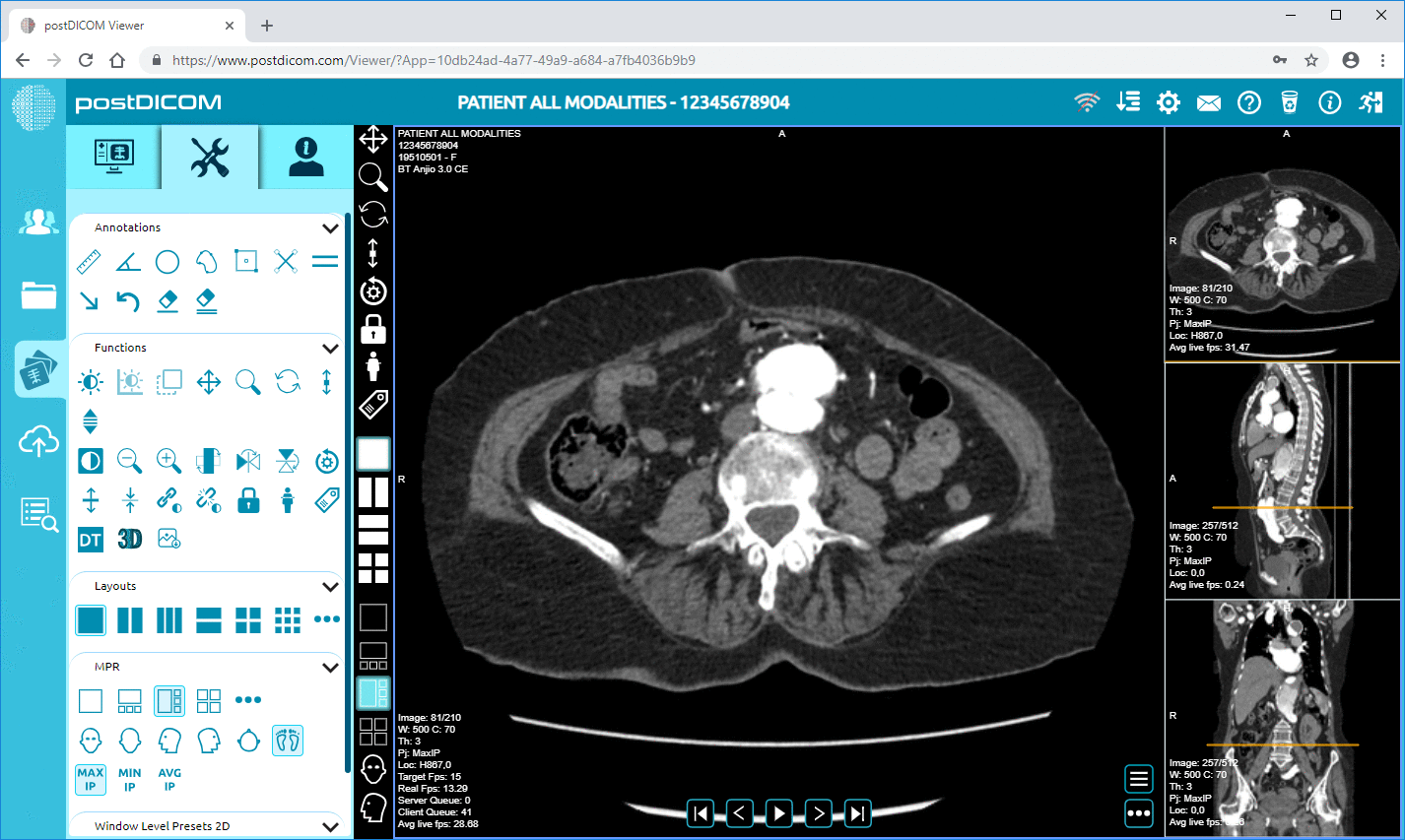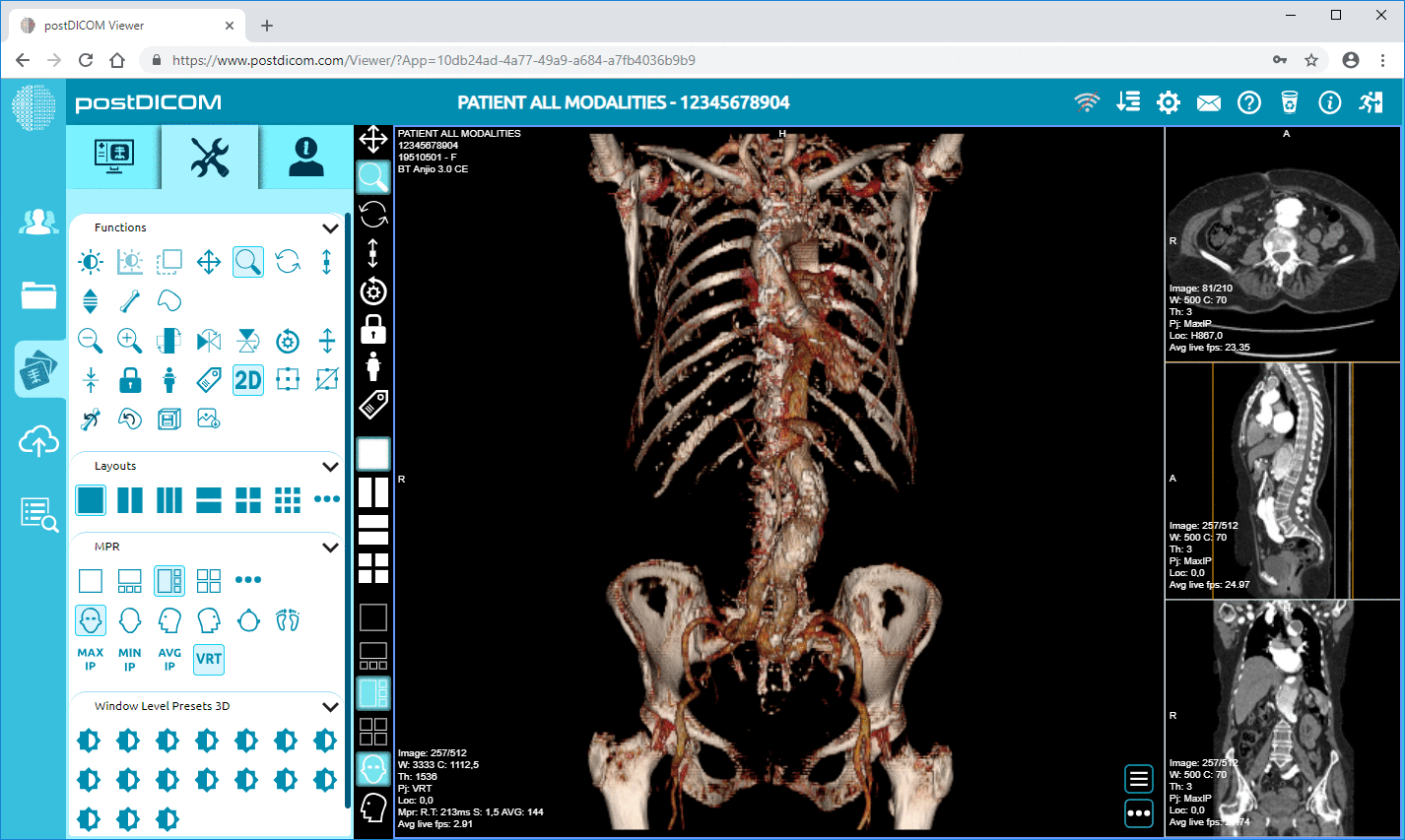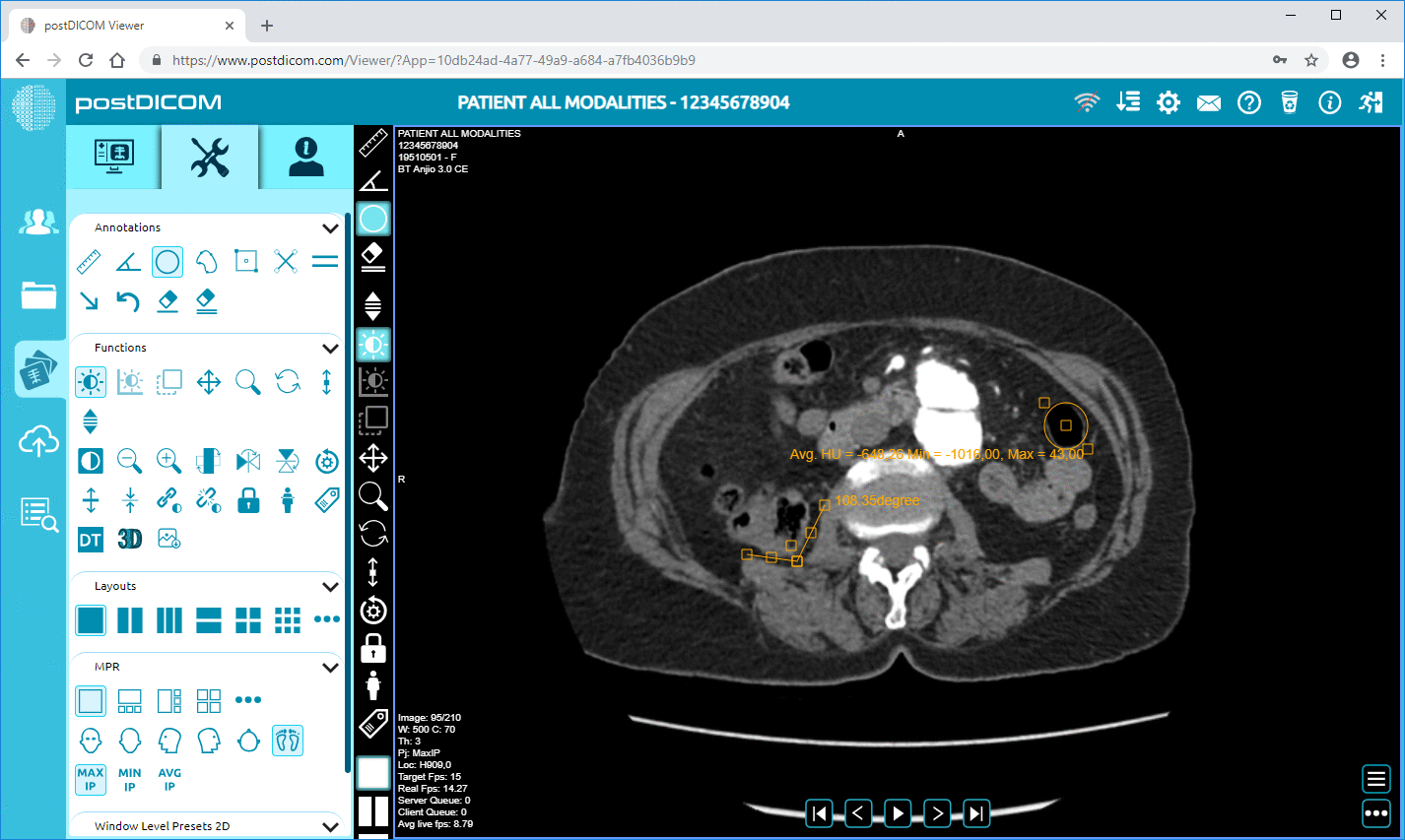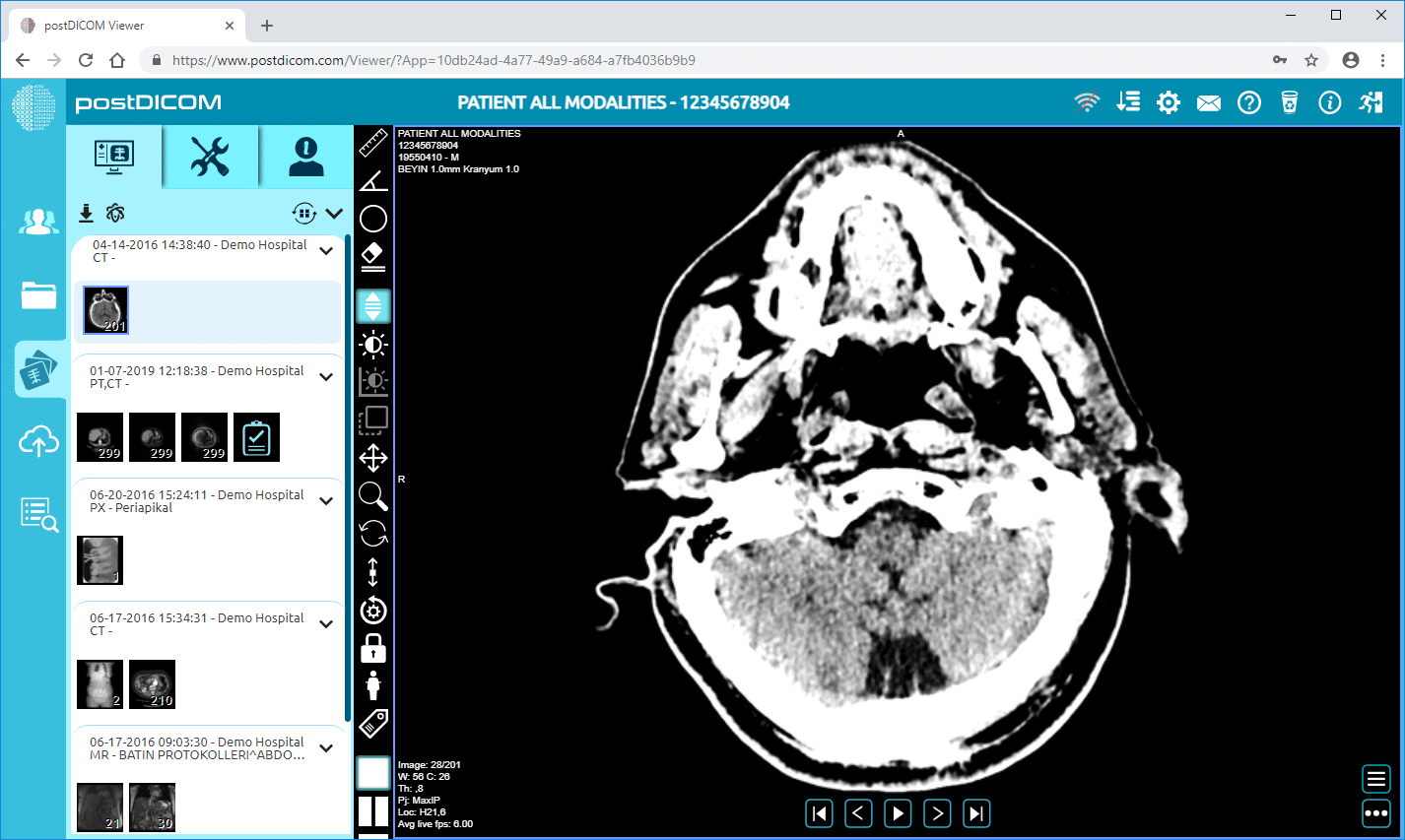
DICOM controls the medical imaging information exchange. DICOMweb enables the web access and integration of imaging capabilities to EHRs by extending DICOM towards RESTful APIs.
Imaging integration is one of the most complicated interoperability situations in healthcare IT.
 - Created by PostDICOM.png)
1. Within Ehr, A Physician Makes An Imaging Order.
2. Order Submitted To The Imaging System Through Hl7.
3. Pacs Imaging Study Carried Out And Maintained.
4. The Radiology Report Was Sent Back Through The Fhir Diagnosticreport Resource.
5. The Imagingstudy Resource Will Be Connected With The Dicomweb Viewer Within Ehr.
Clinical documentation and imaging interpretation are integrated in this workflow.
| Feature | Legacy HL7 Interface | FHIR API Integration |
| Real-time access | Limited | Yes |
| Web-native architecture | No | Yes |
| Scalability | Moderate | High |
| Cloud compatibility | Limited | High |
| Third-party app embedding | Rare | Supported |
Modern healthcare systems increasingly prioritize API-driven architectures for scalability and flexibility.
Interoperability does not reduce security - it enables more powerful administration.
New integration models include:
• Oauth2 Authentication
• Smart-on-fhir Authorization Strata.
• Tls Encryption
• Role-based Access Control
• Comprehensive Audit Logs
The concept of security has to be designed alongside interoperability, rather than treated as a secondary concept.
Vendors should be asked by healthcare organizations:
• Does The System Have A Complete Fhir Api?
• Does It Support Imaging Integration With Dicomweb?
• Embedding Safe Third-party Applications?
• What Are Api Rate Limits?
• What Is The Reconciliation Of Patient Identity?
• Does It Have Publicly Available Documentation?
Such queries differentiate a scalable structure and a closed structure.
The architecture of PostDICOM is expected to operate in interoperable environments. It facilitates:
• Uninterrupted Access To Imaging Studies In Ehrs.
• Integration Of Reports In The Structure.
• Interoperability In Workflow Continuity.
• Flexibility In Neutral Deployment By Vendors.
Instead of substituting EHR systems, interoperable imaging infrastructure enhances the clinical value of EHR systems.
The EHR systems present significant clinical and operational advantages. But their long-term value is not based on documentation features but on integration ability.
Healthcare organizations considering EHR systems must focus on interoperability, API opportunities, and adherence to standards to achieve sustainable expansion, enhanced care coordination, and infrastructure capable of supporting white-collar growth.
A digital silo is an EHR that cannot be closely integrated. Interoperable EHR is a strategic resource.
1) What is the biggest disadvantage of EHR systems?
The total cost of ownership, not necessarily licensing, but implementation, training, disruption of workflow, upgrades, and maintenance of the IT facility, is often the largest disadvantage. Practices tend to underestimate the cost of integration and data migration, particularly when linking the EHR to imaging, lab, and billing systems.
2) Why is interoperability important in EHR systems?
It is due to interoperability that an EHR does not turn into a data silo. By having systems that can share data with reliability, clinicians will have greater availability to complete patient history across the providers, departments, and tools (including imaging). This enhances coordination, minimizes redundant tests, and helps in continuity of care.
3) What causes interoperability problems between EHR systems?
The typical reasons are vendor specific data model, a lack of API coverage, incomplete coverage of standards, inconsistent coding of terminology, and poor system-to-system identity matching. Although it is possible to share data, it might not be reliably understood unless it is semantically interoperable.
4) How do EHR systems integrate with PACS and medical imaging platforms?
Integrating the combination of ordering and results workflows with imaging access is usually referred to as integration. Orders can be relayed via messages (e.g., HL7), and formal clinical information can be shared via APIs (e.g., FHIR). Access to imaging can be provided as an embedded viewer and imaging interface protocol (e.g., DICOM/DICOMweb), depending on the platform.
5) Is FHIR required for EHR integration?
FHIR is no longer universally mandatory, yet it has become a highly popular standard for healthcare integration due to its web-native, API-first nature. Good FHIR integration support systems tend to be easy to build, maintain, and scale more than older, interface-heavy systems tended to be.
6) What should a practice check before choosing an EHR to avoid integration issues?
The important checks here are whether or not the vendor adheres to relevant interoperability standards, they are offer usable API documentation, they are offering stable versioning and rate limits, they are providing secure authorization (where applicable: OAuth2/SMART patterns) and the ability to integrate with imaging workflows in a manner such that clinicians do not need to switch systems to gain access to studies and reports.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |